www.apjph.comwww.apjph.com

Ref Number = ASPR0052
Diagnostic Evaluation for IBD in Pediatric Patient
Muzal Kadim Gastrohepatolgy Division, Child Health Department, University of Indonesia
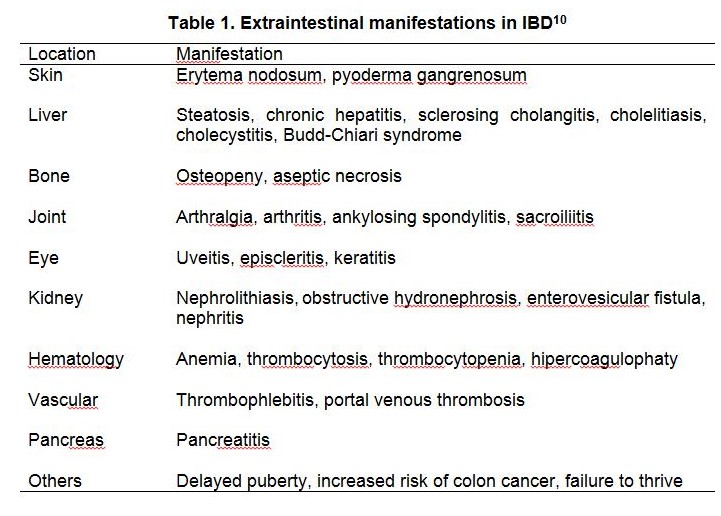
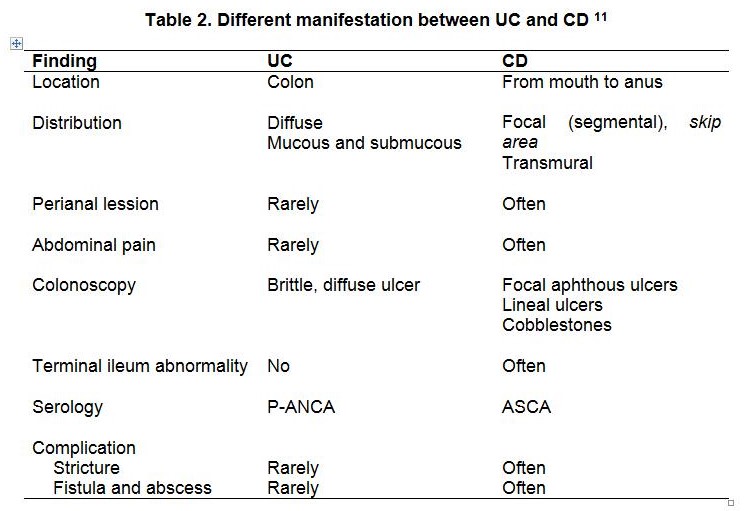
Inflammatory bowel disease (IBD) comprises primarily 2 disorders: ulcerative colitis (UC) and Crohn?s disease (CD). The hallmark of IBD is chronic, uncontrolled inflammation of the intestinal mucosa, which can affect any part of the gastrointestinal tract.1-3 Inflammatory bowel disease affects approximately 1.4 million Americans, and its peak onset is in persons 15 to 30 years of age. 4-6 In a Japanese nationwide survey, the peak age of onset was 20?29 years for UC and 15?24 years for CD, whereas the median age of diagnosis in a Korean study was 35 years. In the study from Hong Kong and China the mean age of diagnosis of CD was 33.1 years and 37.2 years, respectively. Similarly, in a more recent review from China, the mean age of CD was 37.7 years, and 44.0 years for UC. There is some weak and inconclusive evidence of a bimodal age of onset of IBD in Asian patients. Several recent Asian studies confirm that the incidence and prevalence of both ulcerative colitis (UC) and Crohn?s disease (CD) are lower than that in North America and Europe. While this is true, Asia is a very diverse continent and marked differences have been reported in various geographic areas, and an increased incidence and prevalence of IBD are seen in this region 7-9 Diagnosis of IBD poses two major problems. One is the lack of a gold standard, represented by histological or serological confirmation; the second is the number of conditions that mimic IBD and require to be considered in the differential diagnosis. The diagnosis of IBD is established through a global assessment of the clinical presentation, radiographic, endoscopic and pathologic findings.10 Extraintestinal manifestations can occur in 25-35% of cases, as shown in Table 1. Fever as a systemic symptom is usually found in more severe cases. Sometimes these extraintestinal systemic symptoms are more prominent and become the initial symptoms of IBD patients, before gastrointestinal symptoms occur. So that the diagnosis is unthinkable from the start.1012 ASPR0052 - 1 Diagnosis of IBD made by the history, physical examination, and other investigation. The IBD working group of the European Society for Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) establishes diagnostic criteria known as Porto criteria. The possibility of IBD should be considered if in history taking there is a complaint of diarrhea accompanied by abdominal pain and persistent weight loss (> 4 weeks) or recurring (> 2 episodes in 6 months). Suspicion increases if there is a family history of IBD. Anemia, thrombocytosis and increased ESR, are the three most commonly found laboratory results. Endoscopic examination (colonoscopy/ gastroscopy) and histopathology are important for establishing the diagnosis of IBD and distinguishing between UC and CD.13 Currently there is a specific serological examination method to distinguish UC and CD, such us perinuclear anti-neutrophilic cytoplasmic antibody (P-ANCA) and anti-Saccharomyces cerevisiae-antibodies (ASCA). P-ANCA examination is generally positive in patients with UC while ASCA is specific for CD.12,14 However, some experts consider this examination unnecessary because there is not much benefit in establishing a diagnosis of IBD, but only to distinguish UC and CD.15 Even Sabery et al found an increase in ESR and anemia more specific and sensitive as an IBD screening test than serological. 16,17 Crohn's disease and ulcerative colitis often have relatively similar clinical features. Symptoms can be either intestinal symptoms or extraintestinal symptoms. Table 2 shows some findings that can distinguish between UC and CD.11 ASPR0052 - 2 Ulcerative colitis and Crohn's disease are chronic diseases that often recur and require life-long treatment, therefore both diseases must be evaluated continuously based on their disease activity. Classification of ulcerative colitis activity was first published by Truelove and Witts in 1955.18 After many classifications of UC disease activity were published, including the Powell-Tuck Index, Mayo-Clinic Score, Rachmilewitz Index, and Lichtiger Score19-22, it turns out that the classification that is more widely used in adult patients has many shortcomings when used in children, so in 2004 in the 'IBD Clinical Trial workshop' in America it was agreed that the Pediatric Ulcerative Colitis Activity Index (PUCAI) is a good classification for children. 23 Crohn's disease activity index was first published in 1976 by Best et al.24 The classification also appeared to have many weaknesses so that in 1980 Harvey and Bradshaw published a better and easier classification called Harvey-Bradshaw Crohn's disease activity index.25 IBD management aims to relieve symptoms, prevent recurrence, maintain quality of life and ensure adequate nutrition so that children can achieve optimal growth and development. The management of IBD includes pharmacotherapy, nutrition, and surgery. Pharmacotherapy in IBD can be divided into 6 categories, namely aminosalicylate, corticosteroids, immunomodulators, antibiotics, probiotics and biological agents. The use of these drugs depends on the type of IBD and the severity of the disease.11,12 Several alternative therapies such as cyclosporine, methotrexate, heparin, interferon type 1, and tacrolimus have been studied and published.26-30 Azathioprin is one of the second-line drugs that has been proven effective for patients with UC and CD.31,32 In addition, in cases of moderate to severe ulcerative colitis that have been refractory to conventional anti-TNF- (Infliximab) therapy have been shown to be effective in remission and maintenance induction.33,34
Keywords: IBD, UC, CD, P-ANCA, ASCA
Refference:
1. Haggit RC. Differential diagnosis of colitis. Dalam: Goldman H, penyunting. Gastrointestinal pathology. Baltimore: Wlliams & Wilkins,1998. h 325-52. 2. Seidman E. Inflammatory bowel disease. Dalam: Sleisenger MH, Fordtran JS, penyunting. Gastrointestinal disease. Philadelphia: WB Saunders, 1989. h 417-91. 3. Kugathasan S, Judd RH, Hoffman RG, Heikenen J, Telega G, Khan F, Weisdorf-Schindele, et al. Epidemiology and clinical characteristics of children with newly diagnosed inflammatory bowel disease in Winconsin: A statewide population based study. J Pediatr.2003;143:525-31. 4. Hanauer SB. Inflammatory bowel disease:epidemiology, pathogenesis and therapeutic opportunities. Inflamm Bowel Dis.2006;12:S3-9. 5. Abraham C, Cho JH. Inflammatory Bowel Disease. New England Journal of Medicine.2009;361:2066-78. 6. Jenkins HR. Inflammatory bowel disease. Arch Dis Child.2001;85:435-7. 7. Lee YM, Fock KM, See SJ, Ng TM, Khor C, Teo EK. Inflammatory bowel disease and racial differences. Racial differences in the prevalence of ulcerative colitis and Crohn?s disease in Singapore. J Gastroenterol Hepatol.2000;15:622-5. 8. Yang SK, Hong WS, Min YI, Kim HY, Yoo JY, Rhee PL, et al. Kolitis ulseratif. Incidence and prevalence of ulceratve colitis in the Songpa-Kangdong district, Seoul, Korea, 1986-1997. J Gastroenterol Hepatol.2000;15:1037-42. 9. Ahuja V, Tandon RK. Inflammatory bowel disease in the Asia-Pacisific area: a comparison with developed countries and regional differences. J Dig Dis.2010;11:134-47. 10. Lakatos PL, Fischer S, Lakatos L, Gal I, Papp J. Current concept on the pathogenesis of inflammatory bowel disease-crosstalk between genetic and microbial factors: pathogenic bacteria and altered bacterial sensing or changes in mucosal integrity take "toll"? World J Gastroenterol.2006;12:1829-41 11. Hyams JS. Inflammatory bowel disease. Pediatr Rev.2005;26:314-20. 12. Hendrickson BA, Gokhale R, Cho JH. Clinical aspects and patophysiology of inflammatory bowel disease. Clin Microbiol Rev.2002;15:79-94. 13. IBD working group of the European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN). Inflammatory bowel disease in children and adolescents: recommendations for diagnosis the Porto criteria. JPGN.2005;41:1-7. 14. Canani RB, de Horatio LT, Terrin G, Romano MT, Miele E, Staiano A, et al. Combined use of noninvasive test is useful in the initial diagnostic approach to a child with suspected inflammatory bowel disease. JPGN.2006;42:9-15. 15. Danese S, Fiocchi C. Ulcerative Colitis. New Engl J Med.2011;365:1713-25. 16. Sabery N, Bass D. Use of serologic markers as a screening tool in inflammatory bowel disease compared with elevated erythrocyte sedimentation rate and anemia. Pediatrics.2007;119:e193-9. 17. Ouyang Q, Tandon R, Goh KL, Pan GZ, Fock KM, Fiocchi C, Lam SK, Xiao SD. Management consensus of inflammatory bowel disease for the Asia?Pacific region. J Gastroenterol Hepatol. 2006;21(12):1772-82. 18. Truelove SC, Witts LJ. Cortisone in Ulcerative colitis; final report on a therapetic trial. Br Med J.1955;2:1041-8. 19. Powell-Tuck J, Bown RL, Lennard-Jones JE. A comparison of oral prednisolone given as single or multiple daily doses for active proctocolitis. Scand J Gastroenterol. 1978;13:833-7. 20. Shutterland LR, Martin F, Greer S, Robinson M, Greenberger N, Saibil F, Martin T, Sparr J, Prokipchuk E, Borgen L. 5-Aminosalicylic acid enema in the treatment of distal ulcerative colitis proctosigmoiditis, and proctitis. Gastroenterology. 1987;92:1894-8. 21. Rachmilewitz D. Coated mesalanine (5-aminosalicylic acid) versus sulphasalazine in the treatment of active ulcerative colitis: a randomised trial. BMJ. 1989;298:82-6. 22. Lichtiger S, Present DH. Preeliminary report: cyclosporin in treatment of severe active ulcerative colitis. Lancet. 1990;336:16-9. 23. Turner D, Otley A, deBruijne J, Mack D, Uusoue K, Zachos M, Mamula P, Hyams J, Griffiths AM. Development of a pediatric ulcerative colitis activity index (PUCAI). J Pediatr Gastroenterol Nutr.2006;43:E47. 24. Best WR, Becktel JM, Singleton JW, Kern F Jr. Development of a Crohn?sdesease activity index. National Cooperative Crohn disease Study. Gastroenterology.1976;70:439-44. 25. Harvey RF, Bradshaw JM. A simple index of Crohn`s disease activity. Lancet.1980;1:514. 26. Shibolet O, Regushevskaya E, Brezis M, Soares-Weiser K. Cyclosporine A for induction of remission in severe ulcerative colitis. Cochrane Database Syst Rev.2005;2005:CD004277. 27. Chande N, MacDonald JK, McDonald JWD. Methotrexate for induction of remission in ulcerative colitis. Cochrane Database Syst Rev.2007;4:CD006618. 28. Chande N, McDonald JWD, MacDonald JK. Unfractionated or low-molecular weght heparin for induction of remission in ulcerative colitis. Cochrane Database Syst Rev.2008;2:CD006774. 29. Seow CH, Benchimol EI, Griffiths AM, Steinhart AH. Type I interferons for induction of remission in ulcerative colitis. Cochrane Database Syst Rev.2008;3:CD006790. 30. Baumgart DC, MacDonald JK, Feagan BG. Tacrolimus (FK506) for induction of remission in refractory ulcerative colitis. Cochrane Database Syst Rev.2008;3:CD007216. 31. Ardizzone S, Maconi G, Russo A, Imbessi V, Colombo E, Porro GB. Randomised controlled trial of azathioprine and 5-aminosalicylic acid for treatment of steroid dependent ulcerative colitis. Gut.2006;55:47-53. 32. Fraser AG, Orchard TR, Jewell DP. The efficacy of azathioprine for the treatment of inflammatory bowel disease: a 30 year review. Gut.2002;50:485-9. 33. Rutgeerts P, Sandborn WJ, Feagan BG, Reinisch W, Olson A, Johanns J, et al. Infliximab for induction and maintenance therapy for ulcerative colitis. New Engl J Med.2005;353:2462-76. 34. Lawson MM, Thomas AG, Akobeng AK. Tumour necrosis factor alpha blocking agents for induction of remission in ulcerative colitis. Cochrane Database Syst Rev.2006;3:CD005112.
Disclaimer: The Views and opinions expressed in the articles are of the authors and not of the journal.
Editor-In-Chief
Journal Office
Mid City Hospital, 3-A Shadman II
Jail Road, Lahore ,Pakistan
Mid City Hospital, 3-A Shadman II
Jail Road, Lahore ,Pakistan
Managing Editor
Dr. Intan Juliana Abd Hamid
Support & Help
Support & Help
Assistant Editor
Dr. Sadia Shabbir Hussain
Support & Help
Support & Help
Digital Content Editor
Dr. Khalid Masud
Administrator
Administrator